Pregnancy is a challenging time for women that causes significant changes in their bodies. Among the many changes is the fluctuation in hormone levels. The thyroid is a butterfly-shaped gland located at the base of the neck that produces thyroid-stimulating hormone (TSH).
Thyroid hormones control how your body uses energy, affecting how nearly every organ in your body works—even how your heart beats. Due to the increased demand for this hormone by both the mother and baby during pregnancy, it leads to the overproduction or underproduction of TSH, called gestational thyroid imbalance.

Types of Thyroid Imbalance
This overproduction and underproduction of TSH hormones is called Hyperthyroidism and Hypothyroidism.
- Hyperthyroidism: Hyperthyroidism is an overactive thyroid gland that produces too much thyroid hormone.
- Hypothyroidism: Hypothyroidism occurs when the thyroid gland is underactive and produces too little thyroid hormone.
Both hyperthyroidism and hypothyroidism can have significant health impacts if not appropriately managed. Pregnant women with thyroid disorders need to receive regular medical attention to manage their hormones.
Diagnosis and Symptoms of Gestational Thyroid Imbalance
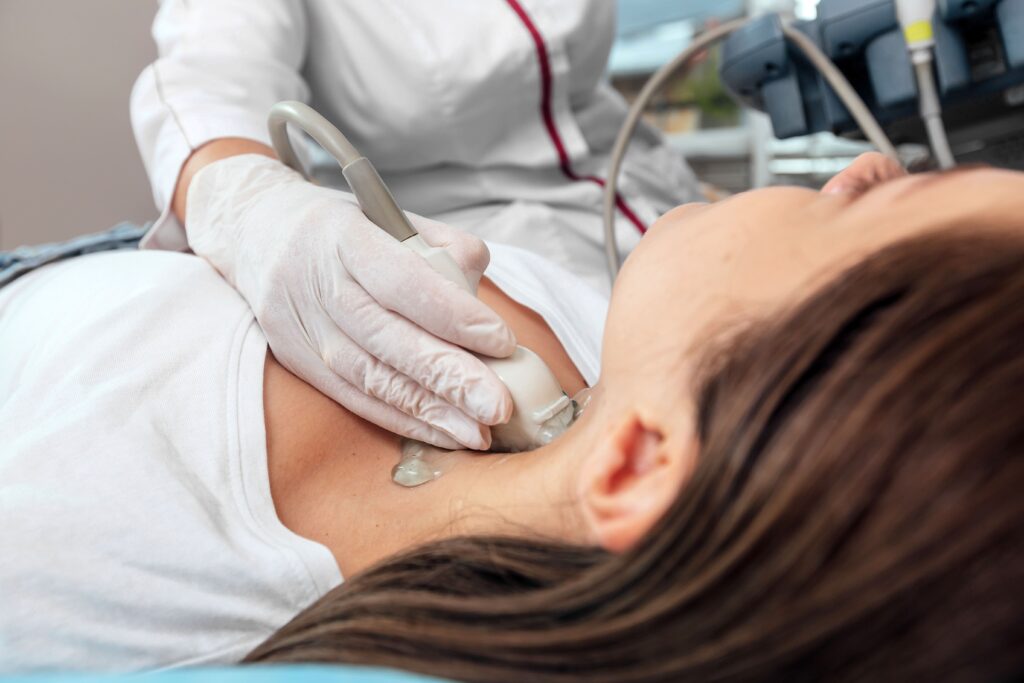
Your healthcare provider conducts a physical exam and a blood test to check for thyroid conditions. The blood test measures the levels of thyroid hormones and thyroid-stimulating hormone (TSH) in your body. TSH is a hormone that signals your thyroid gland to produce thyroid hormones.
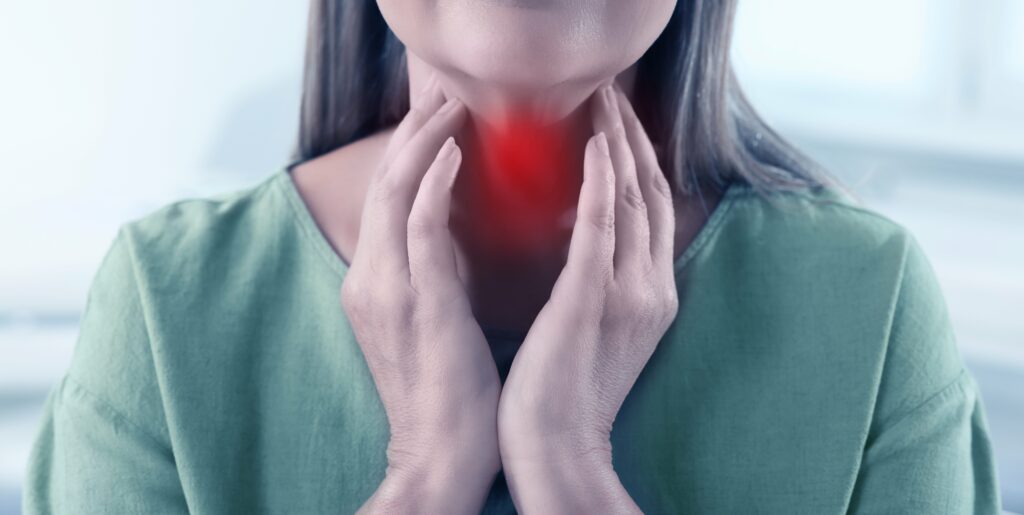
Some of the common symptoms of Gestational thyroid imbalance are:
- Hoarse voice
- Low tolerance to cold temperatures
- Dry skin and hair
- Carpal tunnel syndrome
- Fatigue
Sometimes, these symptoms overlap with typical pregnancy symptoms, so detecting them as early as possible is vital. Additional signs to watch for are:
- Weight gain
- Constipation
- Muscle weakness
Risks of Hypothyroidism and Hyperthyroidism to the mother
- Mild hypothyroidism in most expecting mothers might be unaffected and have no symptoms at the onset of pregnancy. If left undiagnosed, severe hypothyroidism can lead to anaemia, lack of thyroid function, risks of miscarriages, stillbirth or preterm birth, underweight babies and other significant concerns due to this condition.
- Hyperthyroidism in pregnancy may be present initially but might be diagnosed later, around the second trimester. Inadequately treated hyperthyroidism leads to premature labour and preeclampsia.
Risks of maternal Hypothyroidism and Hyperthyroidism to the baby
Thyroid hormones are an integral source for the overall development of a growing fetus. It mainly facilitates the development of the brain and the spinal cord. Hypothyroidism and hyperthyroidism must be diagnosed early in your pregnancy, and once diagnosed, it is crucial to follow the treatment plan and medication suggested by your endocrinologist.
Treatment and Prevention
- Medical Care: Your obstetrician will refer you to an endocrinologist, who will recommend supplements or medications, treatment plans, and regular follow-ups.
- Dietary recommendations: Your doctor will advise you on specific dietary changes. It is essential to eat a variety of nutritious foods and stay well-hydrated. Regular physical activity and proper meal planning can also support your thyroid health.
Postpartum
Postpartum thyroid hormone levels tend to fluctuate and might worsen later, usually three months after the birth of your baby, due to discontinued prescribed thyroid supplementation and neglect in monitoring thyroid function. Hence, your endocrinologist will advise a high dosage of thyroid medications or supplements and serum TSH tests in such cases.
Regular monitoring and treatment, guided by an endocrinologist, are essential to ensure a healthy pregnancy and postpartum period. With proper care, women with gestational thyroid imbalances can effectively support their health and the development of their growing baby.