Preeclampsia is a pregnancy-related disorder characterized by high blood pressure and damage to organs, typically the liver and kidneys. It usually occurs after the 20th week of gestation and can pose risks to both the mother and the unborn baby. While the exact cause of preeclampsia remains unknown, several factors such as genetics, immune system dysfunction, and inadequate blood flow to the placenta are thought to contribute to its development.
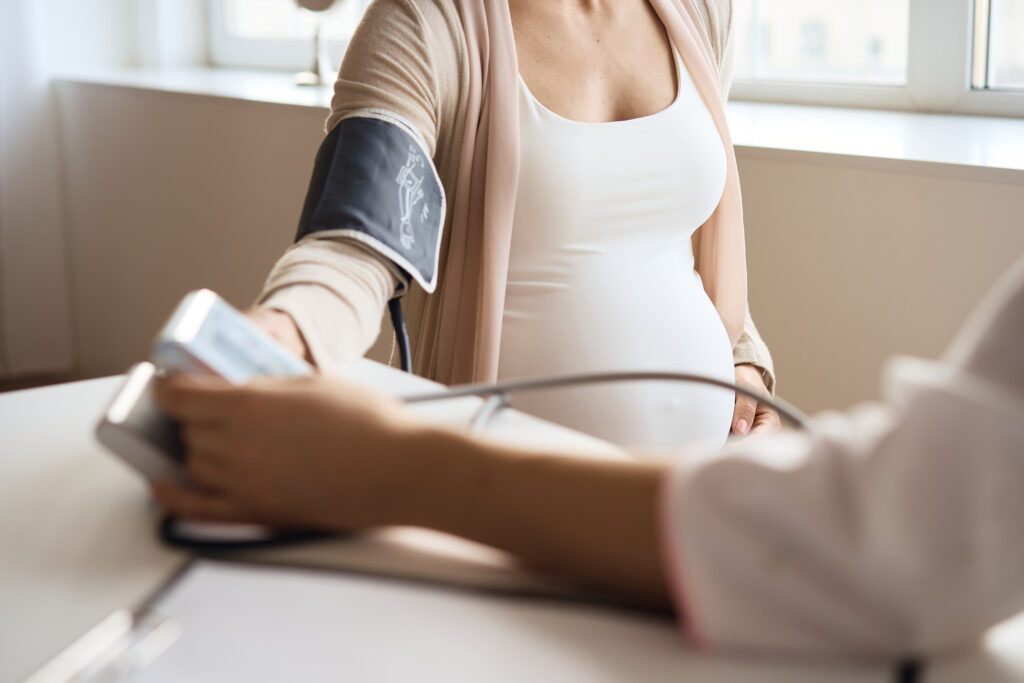
Signs and Symptoms
Recognizing the signs and symptoms of preeclampsia is crucial for early detection and management.
Common symptoms include:
- Persistent high blood pressure
- Swelling in the hands and face
- Sudden weight gain
- Headaches
- Changes in vision
- Abdominal pain
Additionally, protein in the urine, often detected during routine prenatal check-ups, is an important diagnostic marker of preeclampsia. It’s vital for pregnant women to communicate any unusual symptoms to their healthcare providers promptly.
While preeclampsia can affect any pregnant woman, certain risk factors increase the likelihood of developing this condition. These include a history of preeclampsia in previous pregnancies, high blood pressure, obesity, multiple pregnancies (twins, triplets, etc.), and certain underlying health conditions like diabetes or kidney disease. Although prevention is challenging, regular prenatal care, a healthy lifestyle, maintaining a balanced diet, staying physically active, and adhering to the prescribed prenatal vitamin regimen can help reduce the risk and severity of preeclampsia.
Preeclampsia is a potentially serious pregnancy complication that requires careful attention and management. Early detection and appropriate prenatal care are essential to ensure the well-being of both mother and baby.
By understanding the signs, risk factors, and preventive measures, expectant mothers can work closely with their healthcare providers to navigate preeclampsia and achieve a healthy pregnancy outcome.
For more information, please consult our team of Obstetricians. To book an appointment, call 1800 419 1397.